Definition of the Problem
Introduction
Risk management (RM) has been defined as the process of “planning, organizing, leading, and controlling the activities of the organization in order to minimize the adverse effects of accidental losses on that organization at reasonable cost. Risk avoidance involves eliminating all losses associated with a particular activity, loss prevention involves reducing the chance of a mishap occurring, and loss reduction emphasizes reducing the severity and impact of losses once they occur. Loss prevention techniques focus on reducing the frequency of occurrences likely to result in claims and/or lawsuits.
In health care, risk management has become an important issue during the 1980’s and 1990’s. The complexity of the legal environment has challenged institutions to strengthen the practice of health care to protect staff and hospitals from loss. Risk management is defined as the “science for identification, evaluation, and treatment against the risk of financial loss. Risk management also envisages the evaluation and scrutiny of medical treatment to identify and circumvent injuries to patients.
What risk management is about?
RM is concerned with utilizing key functional activities of the organization in order to reduce the detrimental effects of accidental losses on that organization at prejudged and predetermined costs. Further, the scope of risk management could also be extended to include aspects of recognizing, assessing and protecting against the risks of financial losses that may arise due to risk materialization.
Further, there have been paradigm shifts in the underlying causes of fundamental issues governing risks in patient management. While at one time, the safeguards against losses or damages to the financial strengths of health care institution and the prevalence of a reliable treatment environment were considered paramount, this has now shifted in terms of greater need for preventing harm and injury to patients by offering them a greater degree of health care protection and adequate safeguards against injuries caused by neglect by concerned health care professionals.
Thus, it could be seen that over time, the onus has shifted from the health care organization’s need to protect its own health care environment from outside malpractices attacks, to a more focused and perhaps narrower need to keep the best health care interests of the patient uppermost and to better the quality of service and discharge all responsibilities vested upon the health care workers, which, it is believed would significantly reduce the aspects of medical malpractices and issues connected therewith.
The industry’s risk manager of today faces many new and exciting challenges. By conventional practices, the job revolves on safeguarding pecuniary trust of the organization and preserving a secure milieu. Today, the focus has broadened to include preventing patient injury and improving the quality of service. The administrator and physician must now respond and increase the emphasis on a system that can monitor, promote and guarantee the quality of service. Their goal is to reduce malpractice verdicts, cut defense costs, and control the insurance premium (Youngberg, 1990).
Background of the problem
The underlying causes of the increase in malpractice claims were not addressed. The causes included technology advances in medicine, which carry increased risk of injury, deterioration of the physician-patient relationship, and patient’s unrealistic expectations as to treatment outcomes.
The likelihood of errors increased due to the increased numbers of individuals involved in patient care. Risk management is primarily designed to protect the financial assets of an organization by assuring adequate financial protection against potential liability through appropriate insurance coverage, reducing liability when untoward events occur, and preventing those that are most likely to lead to liability (Huffman,1990).
The word ‘liability ‘is used in various ways, but general definition would be the state of being exposed to damage, danger, expenses, etc. Hospital’s professional liability is an area of great risk and all hospitals must make decision on the amount of coverage they will carry. Comprehensive loss and exposure information must be collected and the data analyzed prior to purchasing insurance coverage. In an effort to ease the malpractice crisis, state legislators enacted a variety of laws designed to establish limits on the amount of awards, set up arbitration screening panels, revise the contingency fee systems, and modify the collateral source rules.
Problem statement
Medical malpractice received a great deal of attention in the early 1970’s when a crisis emerged due to the lack of availability of liability insurance. Most insurance carriers increased premiums at alarming rates, and others stopped writing malpractice coverage altogether, thereby shrinking market capacity. The increased frequency and severity of malpractice claims were the primary factors precipitating these actions. Insurers found themselves unable to adequately predict the frequency of claims or to adequately price this line of insurance.
Purpose of the study
Purpose of study
It is proposed to consider the aspects of medical malpractices in a closed environment of the William Beaumont Hospital physicians in Royal Oak, Michigan.
Research Questions
- Whether trusted methods are available that could identify specific medical outcomes of medical malpractices or liability incurring thereon?
- Extent to which risk management and risk managers could make differences.
- Could gaps in physician-patient relations impact upon medical malpractice?
- Could a collapse in communication in a physician-patient relationship result in a malpractice case?
- How could physicians avoid diagnostic errors and law suits?
To prevent loss suits against hospitals and to prevent further injuries to the patients, ensure compliance with state insurance departments. Risk managers must develop a close working relationship with the persons who provide hands-on patient care. These professionals are often the first to realize that an untoward event has occurred. Risk managers must establish an open line of communication so that he or she is advised of events as soon as possible. Risk managers must develop an occurrence reporting system that these professionals understand and are willing to utilize.
Assumptions/Limitations
The study subject will be limited to William Beaumont Hospital physicians in Royal Oak, Michigan.
Definitions
Summary
Risk Management has become a growing concern of all hospital administrators since the 1970’s. Whether the institution is for profit or not for profit, it must be protected from loss to remain competitive in the health care industry. A program must be established, personnel must be educated, legal strategies must be planned, and insurance protection must be ensured. The goal is to provide quality service to the patient and to avoid negligence. The hospitals should be a safe place, not a hazardous environment that creates further injury.
Literature Review
The industry’s risk manager of today faces many new and exciting challenges. Traditionally, the job centered on ensuring financial integrity of the institution and maintaining a safe environment. Today, the focus has broadened to include preventing patient injury and improving the quality of service. The administrator and physician must now respond and increase the emphasis on a system that can monitor, promote and guarantee the quality of service. Their goal is to reduce malpractice verdicts, cut defense costs, and control the insurance premium (Youngberg, 1990).
One of the first steps to determine the severity of action to be taken was to conduct a study of the crisis and possible solutions. President Richard Nixon directed a study in 1971 which was conducted by the Department of Health, Education, and Welfare Secretary’s Commission. The secretary found that malpractice claims were primarily the results of patient injury and adverse results of medical care and treatment.
Some of the findings showed normal circumstance within the study, but not all injuries were due to negligence and not all injuries were preventable. These findings were based on the results of studies concerning the incidence of injuries. More findings proved that the severity of the injury was more apt to be the determining factor in deciding whether a claim would arise. Through these studies, it was concluded that the most effective way to reduce the frequency and severity of injuries was to develop medical injury prevention programs in every health care institution. The American Hospital Association (AHA) gave guidance and it helped promote the acceptance of risk management. According to (Kemshall, 1996) the AHA defined risk management in 1977, “the science for identification, evaluation, and treatment of risk financial loss” and encouraged all hospitals to implement this process as a key solution to malpractice.
The AHA also outlined the basic elements of the program and directed that the manager be someone whose training or background was in hospital administration, insurance, or safety engineering. The AHA guideline also stipulated essential components necessary for an effective program. This description listed mandatory requirements, but left space for modifications that would be dependent upon the unique characteristics of the individual hospital.
The first step in the risk management program would be to gain senior administration support (Youngberg, 1990). It is the governing body of the institution and with the support of administration, staff generally complies. The second step is to designate a risk manager who can coordinate all aspects of the program and to communicate loss prevention activities to key administrators. Next, secure the support of the medical staff and their participation in reporting adverse outcomes, incidents, or any event that may result in a claim. This also includes integration with quality assurance and sharing of information and findings in the monitoring and evaluation of the quality of patient care.
In its simplest form, risk management in health care has historically focused on providing a safe environment for hospital patients. With the formation of health care systems in recent years, the scope of risk management now expands beyond the inpatient setting. Organizations have affiliated components that provide not only acute care hospital but also the out-patient, home care, and long-term care that patients require. The new structure of health care delivery systems brings with it the obligation to increase the scope of risk management. It must extend beyond the acute care hospital to include the organization’s total entities (McGinnis, 1999).
Broadening the focus of patient care is also a risk management initiative. In her publication, Bellandi (1997) emphasizes the importance of recognizing that risk management now means, “…understanding the entire continuum of care and figuring out ways to improve it” 2. Patients may receive a range of care in multiple settings from multiple providers. As hospitals develop new policies and standards of care or update existing ones, they must keep the continuum in constant focus.
An effective risk management program covers all aspects of hospital operations. To achieve this goal, managers must establish early warning systems, targeting clinical areas or practices that present the greatest exposure to liability, and implement preventive action to minimize the risk associated with these activities. Despite the impersonality often prevalent in our society, patients still have high expectations for sympathetic treatment when they visit their physicians (Showalter, 2004). Risk management is primarily designed to protect the financial assets of an organization by assuring adequate financial protection against potential liability through appropriate insurance coverage, reducing liability when untoward events occur, and preventing those events that are most likely to lead to liability (Huffman, 1990).
Liability is used in various ways, but a general definition would be the state of being exposed to damage, danger, expenses etc. Hospital’s professional liability is an area of great risk and all hospitals must make a decision on the amount of coverage they will carry. Comprehensive loss and exposure information must be collected and the data analyzed prior to purchasing insurance coverage.
First, analyze the gross patient service volume, inpatients and outpatients visits, determine the number of employees on staff, full/part-time should be accounted for, any prior loss history and any previous legal expenses paid out are also reviewed. Evaluate loss projections: this can be accomplished in three steps. (1) Determine the frequency and magnitude of loss. The nature of the injury sustained is the best predictor of the value of a loss. (2) Adjust frequency averages to reflect significant future changes in hospital’s risk climate. (3) Review the accuracy of loss payout estimates. This is to include the settlement amount and the cost of the investigation, and defense for both paid and reversed cases. A skilled attorney should be retained for a second opinion as to the estimates of case values.
No one can estimate the amount of coverage an institution should carry, due to the fact that each case differs in each area of care. Youngberg stated that on an average, an annual payout will fall between $100,000-200,000 for justifiable awards in court (Youngberg, 1990). After the data has been analyzed, a risk manager would prepare for the future loss by purchasing insurance. Most hospitals “over kill” the expected loss projection and settle for the purchase of a premium that protects against catastrophic settlements, payoffs which are in millions. Insurance coverage is paid for protection; the risk manager can further protect by ensuring all health care providers work towards preventing loss within the institution.
Risk managers are responsible for developing systems to prevent injuries and other losses within the organization. Performance improvement actions are often initiated in response to suggestions offered by the risk manager. Education is also an invaluable tool in risk management and sometimes is the only activity required to prevent potential safety problems. Risk managers in many healthcare organizations are responsible for developing policies and procedures aimed at preventing accidents and injuries and reducing the organization’s risk exposure (Johns, 2002).
The specific policies and procedures that constitute a risk management program in a hospital are developed in collaboration with the hospital’s legal counsel. Judicial interpretation of statutory law in the court system is a continually evolving process and hospital leadership and governance are well advised to seek the advice of counsel to ensure that risk management practices adequately protect the organization. In general, the infrastructure of a risk management program is designed to (prevent or reduce financial loss, plan for and allocate funds for compensable events, and diminish negative public image resulting from injury claims) (Abdelhak, 1996).
Prevention is a critical aspect of any effective risk-management program. It is important that managers provide the staff with tools to deal with uncomfortable and unfortunate situations, as they will arise frequently due to no fault of the individual staff member (Bleier, 2004).
In summary, risk management has become a growing concern of all hospital administrators since the 1970’s. Whether the institution is for profit or not for profit, it must be protected from loss to remain competitive in the health care industry. A program must be established, personnel must be educated, legal strategies must be planned, and insurance protection must be ensured. The goal is to provide quality service to the patient and to avoid negligent acts. The hospital should be a safe place, not a hazardous environment that creates further negligence.
Sentinel Event Statistics
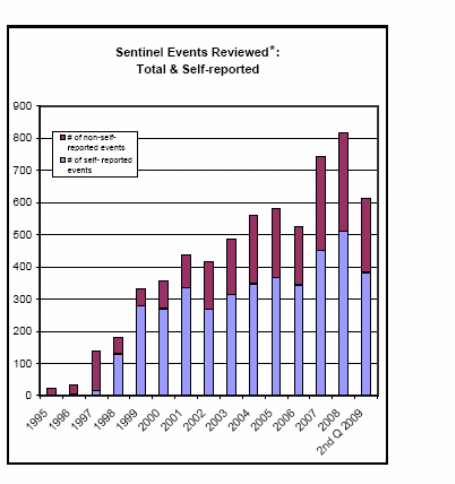
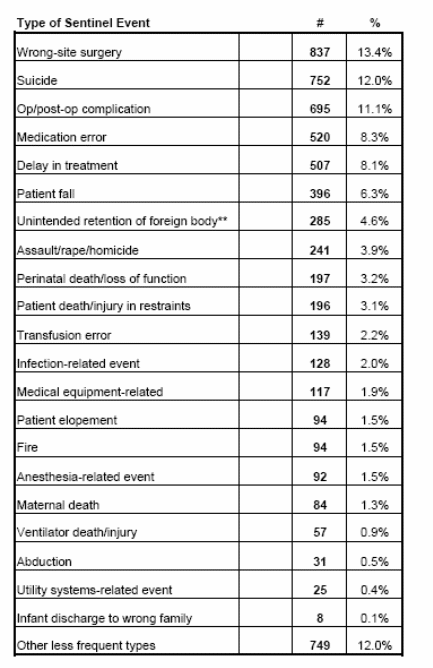
The main aspects that need to be dwelled in this part are preventing those events that have high propensity for attracting liability, or cause for damages in the event of lawsuits. According to the cases reviewed by Joint Commission of Sentinel Event Statistics as of June 30, 2009, there could be many kinds of surgical errors or delays that could harm, or cause death to patients, and thus give rise to criminal or civil proceedings for medical wrongdoing. High on their lists are wrong site surgeries (13.4%), suicides (12%), operative and post-operative complications (11.1%), and delay in treatment (8%) (Sentinel event statistics as of: June 30, 2009, n.d.). (Appendix 1 and 2)
Although it would be presumptuous to blame health care providers for all errors, yet, errors like transfusion errors, errors while administration of injections and anesthesia, ventilator deaths, etc., do come within the purview of providers, and are thus susceptible to legal action, at the behest of the aggrieved party. It is also seen that since 2006, the number of reported cases (self and otherwise) have been rising alarmingly, and year 2008 has witnessed sharp spikes in reporting both total and self-reported cases. The increase in such cases is a cause for major concern since these incidents could trigger off suits of medical malpractices, especially if large scale injury or death is involved.
Omissions and delays
Again, coming to the issue of medical malpractices caused by errors or delay in treatment, in an article written by Sherrie Dulworth in the American Journal of Medical Quality, entitled, “Commentary: Exploiting the Overlap: Using Utilization Management to reduce Medical Malpractice”, the author says that there is need to build pro-active and preventive measures related to omissions and delays in delivery of health care to needy patients (Dulworth, 2003).
Utilization Management and Risk Management
It Is seen that Utilization Management (UM) may be needed to integrate with Risk Management (RM) in order that coverage of both aspects, insurance reimbursements billing, stay in hospitals (typically UM functions) work in harmony with patient omissions and delay in treatments, medical malpractices and its aftermath (typically RM functions). In most settings what is seen is that, due to staff shortages, due weight age for RM functions may not be feasible, given the non- critical nature of its activities, and thus it is necessary that RM and UM co-exist and nourish each other, in order to enhance quality of treatment, eliminate or significantly reduce aspects of high risk medical malpractices and so on.
Medical Malpractices Jury Trial Verdicts
However, it is also seen that if the medical malpractices verdicts of jury are considered, during the calendar year 2008, of the total of nine verdicts, eight have gone in favor of the defendants, and only one has gone in favor of the plaintiff, or the aggrieved party. This was a case involving misdiagnosis, which apparently was settled for an amount of $2,200,000. (Medical malpractice jury trial verdicts (January 1, 2008- December 31, 2008). (n.d.).
It is next necessary to consider the benchmarks that need to be achieved under Operational Risk Management & Safety Assessment (ORM&SA), laid down by Wells Fargo Healthcare Group. The modus operandi for conducting such assessment would be in terms of assessing present compliances and how deficiencies in the present system to make it congruent with desired levels could be achieved. The assessment would also include compliance audits and in-depth questionnaire-aided assessment in major functional areas of health care.
Enterprise Risk Management
Again, Enterprise Risk Management (ERM) forms a major area of public and governmental accountability, including in its scope, management of emergency room, infection control, laboratory, blood bank and transfusion controls. Again, critical areas where risks of medical malpractices could be high are obstetrics, radiology, anesthesiology, and oncology and pain management. This is more sharply accentuated in geriatrics and post and pre-natal interventions.
According to the Wells Fargo Healthcare group, it is necessary that a detailed and comprehensive view of all medical and patient related aspects of patient care be made. According to them, “The purpose of this Operational Risk Management & Safety Assessment (ORM &SA) is to assist an organization in determining how prepared it is to retain risk as well as determine if the care that is provided to the patient meets established standards of care and other recognized benchmarks.” (Wells Fargo Healthcare, n.d.).
Aspects that influence quantum of coverage
There are many aspects that need to be considered while taking up the question of medical malpractices in hospital settings. For one thing, the hospital administration needs to decide upon the amount of coverage that it needs to carry and this has to be laid out on scientific and deterministic basis. For another, the coverage would depend upon a number of variables, which may depend upon controllable and uncontrollable factors. The major aspects that need to be covered would be the gross patients and their service volume, including breakup of inpatients and outpatients statistics. It is also necessary to find out the number of employees, including health care professional whose conduct could impact upon, and make it subject to risks of medical malpractices.
Legal history could dictate future trends
It is evident that before a risk management system is set into place, the history of medical risks and their settlement in the context of the institution needs to be identified and assessed. It is necessary to know cases of previous litigation regarding medical malpractices that have been instituted either against the institution, or against any of its constituent practitioners. If so, it is also important to know how these issues were dealt with and the extent, or quantum of damages that were made by the institution, or its represented insurance agencies, or firms. This aspect is important since this would bring out the public image that is associated with this particular health care center.
Importance of public image in health care settings
It is common knowledge that, to a very large extent, the survival and growth of public health care institutions depend largely upon public image and goodwill that it has earned over years of providing health care services to users. However, even a few instances of medical malpractices by its constituted agents, or health care providers would be enough to earn disrepute, which could significantly impact its image and potential prospects, since few patients would be willing to visit health institutions where the medical services are compromised or neglected, inviting legal complaints and actions. Thus, there are many factors that impinge upon the aspect of medical malpractices, which cannot be seen in isolation but has to be seen in the context of the individual case studies. The importance of a proper methodology for seeking out how best these issues could be addressed to would form the next part of this paper.
Methodology
To prevent loss suits against hospitals and further injuries to the patients, ensure compliance with state insurance departments. Risk managers must develop a close working relationship with the persons who provide hands-on patient care. These professionals are often the first to realize that an untoward event has occurred. Risk managers must establish an open line of communication so that he or she is advised of events as soon as possible. Risk managers must develop an occurrence reporting system that these professionals understand and are willing to utilize.
Occurrences shall be reported, analyzed, trended, and utilized through Intensive Assessment or other review processes to continually improve systems, processes, education and training to reduce/avoid their occurrence. Systems shall be designed for safety, and system failures shall be corrected to reduce the risk associated with human error. Systems shall strive to minimize both the frequency and impact of occurrences. In order to be successful in identifying potential risks in clinical practice, the following components must exist:
- A method to conduct interviews, chart reviews, and inspections of individual department to identify safety hazards as well as risk exposures in clinic care.
- The ability to identify trends and clusters of incidents reported to the risk management department.
- The integration of risk management information with other sources of data designed to identify problems with medical care, such as quality improvement efforts based on review by clinical indicators.
The goal is to provide commitment and support to senior administration and governing body. Designate a risk manager to coordinate all aspects of the program and to communicate loss prevention activities to key administrative personnel. Support of the medical staff and their participation in reporting adverse outcomes, incident, or any event that may result in a claim. Another is integration with quality assurance and sharing of information and findings in the monitoring and evaluation of the quality of patient care. Establish a reporting mechanism to identify unusual incidents, unexpected outcomes or potential risks. Investigate all serious unanticipated or unexpected patient injury. Analyze prospectively and retrospectively risk exposures for trends or patterns. Implement prevention programs to minimize patient injuries or loss. Educate physicians, nurses, and hospital staff to promote awareness of risk management and liability control. Review of new ventures, programs, services, and technology to address the receipt and review of risk management information.
One of the main ingredients of a well designed risk analysis plan is to manifest probable variations in the volume and regularity of unfavorable health results that emanate from various risk management decision choices. It uses chances of occurrences, levels of trust and other manifestations to display irregularities about human health resulting from various decisions. It localizes a subset of one or more choices of determination resulting in its identification of a subset of one or more decision options leading to accepted (for example, randomly not chosen) chances of risk happenings.
Thus, in a research study of this kind, the best method could be in terms of face-to-face interviews with the management and health care professionals, who are the best people to whom the questions during conducted interviews could be directed. It is, therefore, proposed as a part of this methodology, to interview twenty Risk Managers of an institution in order to gain a firsthand knowledge about the present state of medical malpractice in their institutions and how best they, as responsible officials of the institutions, could address such issues. Further, it is also necessary for the research methodology to delve on issues connected with maintenance of health care standards, like negligence, dereliction of duties, criminal liability, and claim settlement and so on.
There are many issues directly and indirectly connected with medical malpractices, like insurance coverage, underwriting, evidence, or rebuttal of claims, and other issues that need to be taken up in the case of risk management. Further, the methods need to consider the role of risk managers as prominent players in the appraisal and evaluation of risk management. The methodology needs to envisage use of interviews, reviewing charts, inspection of individual departments and the degree of safety risks in exposure of clinical care, or its professed underutilization.
Another aspect that needs to be considered is that risk managers need to assess deficiencies in the present system that may give rise to incremental levels of risks, real or assumed. Thus, it is necessary that all types of present risks need to be identified and assessed, as an integral part of risk management in the scope of medical malpractices.
Data Analysis
Introduction
The Joint Commission on Accreditation of Healthcare Organization (JCAHO), an independent organization that evaluates and accredits healthcare organizations and healthcare programs throughout the United States, has recently promulgated patient safety standards that took effect in January 1989. Although JCAHO standards are typically not the driving motivator for risk management activities, the moral and business cases for making these areas of focus central to any risk management strategic plan seems evident. JCAHO provides a good template to create a culture of safety (Youngberg, 1990).
The goal of risk management is to reduce an entity’s accidental loss of corporate assets, personnel, revenue, and reputation. Each organization’s risk management plan should include the following components: the plan’s objectives, key elements, responsibilities, methods, and areas of focus for the current year.
Risk Management Plan
Objectives: The objective of the Regional Medical Center risk management plan is to control and minimize loss in order to protect the assets of the facility and the safety of all staff, patients, and visitors.
Key Elements: Risk management involves several key elements. The methods for implementing these elements are displayed later in this document. The key elements are: identifications of risk issues, evaluation of areas of risk, communication of risk information, education of organizational personnel and others, and reduction of risk.
Responsibilities: The risk manager will be responsible for managing Regional
Medical Center risk management activities. These activities include:
- Coordinating insurance coverage.
- Managing claims against the facility.
- Interfacing with legal counsel.
- Identifying and analyzing areas of risk exposure.
- Analyzing and recommending appropriate risk control techniques.
- Developing and maintaining a data management system.
- Implementing and monitoring safety, training, and quality assurance programs.
- Analyzing, reporting, and monitoring risk management data and information.
Although the risk manager has responsibility for this plan, risk cannot be reduced without education and participation by all team members at Regional Medical Center. All team members are expected to report events, follow standards of practice, identify risk events, guide the organizational mission, implement systems to reduce risks, and budget monies to solve problems (Johns, 2002). Risk managers will be available to consult with any department or manager to assist in a risk assessment of the environment or system. Risk managers will also research issues and gather additional data to assist decision-makers in the search for solutions. This research may include local, state, or national data.
Methods for Carrying Out Key Elements
Identification: The methods of identification include, and are limited to, incident reports, medical device reports, customer comment tracking forms, attorneys’ health records request, security reports, performance improvement referrals, medical staff/peer review reports. Safety hazard reports, supervisor reports, documentation by staff and/or phone conversations with individuals who feel a need to speak about issues, and visual inspection of all areas of the organization in order to identify potential risk situations.
Committee membership and participation are essential for risk identification. Risk managers will attend, when possible, any committee meeting that requests risk management to be present. Risk managers will assist in the credentialing process whenever there is a request or need to do so. Risk managers will research the appropriate databases and assist in obtaining profiles concerning procedures as needed or required by the medical staff bylaws. Risk management will identify high-risk areas due to trends in practice, advanced changes in technology, and national data might highlight potential areas of risk at Regional Medical Center. The high-risk areas at Regional Medical Center are the emergency department, obstetrics, surgery, anesthesia, critical care, and pediatrics.
These areas have the potential for creating situations that can have a significant economic and emotional impact on the organization. Risk management will monitor the off-campus sites by receiving notification of any incidents that occurs off-campus, as well as through periodic visits by the risk manager to each site. Maintaining information is and always will be the foundation of risk management. Most information will be maintained on the computer system for ease of data retrieval, to keep paper to a minimum, and to make record transfers easier and timely.
Regulatory agencies are constantly changing guidelines, regulations, and statutes. The risk manager will monitor changing regulations and assist team members in implementing practice changes pertinent to the regulations. Agencies that may affect the organizations are JCAHO, Health Care Financing Administration (HCFA), state licensing boards, state and federal legislative bodies, and others.
Evaluation: A major role of the risk management department is to continuously evaluate data, systems, process, events, documents, and departments or areas for risk. This can be done through committee participation, reporting mechanisms, such as patient satisfaction, data and incident reports, data trends such as needle sticks and reported medication errors.
The risk management department will complete an investigation of any occurrence and rate the risk of the event. A further investigation will then occur, with priority given to all events that alter an outcome for a patient, a staff member, or a practitioner. The method of investigation will be determined by the event itself but could include data collection and review. Health record review, committee participation, incident report investigation, making rounds in the area, consulting with specialists to assist in the investigation, including other managers, educators, insurance carriers attorneys, law enforcement and finally the process such as root- cause analysis, case study, or peer review to determine what occurred. The leadership staff in the organization will then be responsible for changing processes or improving systems to reduce future occurrences and risk.
The risk analysis will also be reported periodically to the board of directors for its overall direction. The risk management department will maintain confidential records of the analysis, including the progress taken to evaluate processes that may be causing increased risk and the suggested actions for improvement. After the analysis is completed, the action steps will be implemented to solve problems or to improve the outcome for the parties involved. After changes have been made, a periodic evaluation of the success of the change will occur, and the evaluation will be reported to senior leadership.
Communication: Communication of risk management functions, information, data collection, and risk assessment is an important function within the risk management plan. The priority for communication is to inform and educate employees, physicians, customers, and others of risk issues and problem-solving processes. Confidential information will be shared only on a need-to-know-basis without exception. Risk management will determine the confidentiality of certain communication links for direct and discrete information.
Communication may be directed to any or all of the following groups, as deemed appropriate: administration, medical staff, employees, patients, the board of directors, and employees. Communication to the board of directors will be done on a quarterly basis. This communication mechanism will also include performance improvement activities related to the risk management plan.
Education: Education regarding risk management activities, risk reduction, opportunities, and other ways to improve the organization is a key element of the risk management plan. The medical center will also participate in collaboration with the parent organization’s national risk management program through involvement in the Risk Management Incentive Program. Proven measures of risk reduction may result in lowered liability rates. The measures may be in the form of general orientation, root-cause analysis session, special education programs, conferences, medical staff meetings, employee staff meetings, board reports, department rounds and informal discussions. Risk management will be prepared to assist the organization in national regulatory changes that influence how the work is done. Educational opportunities will be sought out in the employee environment to reinforce the principles of risk reduction.
Reduction: The outcome of any effective risk management plan is reduced risk.
The problem-solving process of identification, evaluation, education, and communication will be the mechanism for reducing risk. The reduction of risk will provide a safer environment for patients, staff, providers, and visitors. Each of the activities will identify action steps and personnel required to resolve issues. Problem solving activities and their outcomes will be shared through Areas of Focus in Fiscal Year 2008:
- Timely incident reporting.
- Reduction of medication errors.
- Implementation of workplace violence program.
- Data trending of resuscitation outcomes.
Attention to medical errors escalated over five years ago with the release of the study from the Institute of Medicine (IOM), To Err is Human, which found that between 44,000 and 98,000 Americans die each year in U.S. hospitals due to preventable medical errors. Hospital errors rank between the fifth and eighth leading cause of death, killing more Americans than breast cancer, traffic accidents or AIDS. Serious medication errors occur in the cases of five to ten percent of patients admitted to hospitals. These numbers may understate the problem because they do not include preventable deaths due to medical treatments outside hospitals (Kaiser, 2007). Most often, medication errors can be attributed to one or more of the following:
- Faulty prescribing, monitoring or refilling practices.
- Inappropriate formulas.
- Improper documentation.
- Inadequate communication.
How can physicians avoid diagnostic errors?
Expert physician has to investigate/document all patient complaints. Maintain a comprehensive record of the patient’s history by implementing a template to ensure consistency and thorough evaluation and documentation. Physician should avoid allowing age to become a determining factor in the evaluation of a diagnosis. Review results from a previous diagnostic exam and promptly pursue further diagnostic studies. Also ensure that a diagnostic tracking system identifies delinquent follow-up. Handwriting should be legible and easy to understand. Legibility issues are resolved through the use of electronic prescription ordering and record keeping.
The use of preprinted prescriptions for frequently prescribed compounds is another effective method of providing easily read prescriptions and avoiding illegible orders. Physicians should avoid verbal orders. If verbal orders must be given, physicians should repeat the order, spell the name of the medication, and ask for the order to be repeated to verify understanding. Alternatively, consider the use of fax transmission of prescriptions to the pharmacy to provide a written document which can be maintained in the patient’s chart (JACHO, 2005).
What are the risk exposures and hazards?
Clinical judgment is a risk exposure for physicians. Many factors contribute to a lack of information necessary to support the physician’s clinical decisions about patient care. They include: an incomplete or inaccurate history, over-reliance on a referring physician’s diagnosis without independent assessment, failure to obtain consultation, misinterpretation of diagnostic studies, inadequate office systems to track test results, cognitive bias, inadequate supervision of personnel and inadequate knowledge (MICA, 2002).
How can corrective actions be implemented?
In order to enhance the security aspects for patients and disallowing mistakes, the Government should set up a National compulsory unfavorable occasion reporting system so that health care settings disseminate information that can assist them in correcting wrong systems and procedures. Computer prescriptions could significantly reduce errors in dispensing drugs and medicines.
This would assist doctors in dealing with issues arising out of undecipherable handwritings and by routinely examining for mistakes, or unsuitable drug usage.
In spite of a ruling by the Institute of Medicine during 2006 that preventable medication error costs $3.58 billion annually, just 5% of hospitals have taken concrete steps to check such occurrences. Health care settings could also help by evolving systems that could control work weeks of professionals to diminish errors arising out of tiredness and need for rest.
The Institute of Medicine (IOM) report called for a 50 percent reduction in medical errors by 2004. Unfortunately, it is not possible to quantify the number of errors today, and therefore, impossible to determine if the goal has been met. The number of errors remains high and there are many issues around substandard quality in addition to error. The 1999 IOM report focused primarily on errors in hospitals, but errors occur in other settings, such as ambulatory care and nursing homes (Bleich, 2005).
In 2001, more than one of five Americans reported they or a family member had experienced a medical error. Some researchers believe that the IOM figures regarding medical errors may represent the tip of the iceberg. In 2002, 35 percent of physicians and 42 percent of the public reported errors in their own or a family member’s care. Neither group, however, placed errors among the most important problems in health care.
Hospitals and other health care organizations decrease medical errors by using expertise, improving processes, identifying mistakes that cause damage, and building a customs of security. Studies have shown that Computerized Physician Order Entry (CPOE) is effective in reducing medication errors. It involves entering drug orders directly into a computer system rather than on paper or orally. (Vantage Professional Education, 2006).
The Institute for Safe Medication Practices conducted a study of 1500 hospitals during 2001 and found that about 3 percent of hospitals were increasingly using CPOE. This technology obviates ambiguity in handwriting, decimal points or acronyms. All matters are processed digitally under this system..
Today, most Americans don’t believe the nation’s quality of care has improved. A 2004 study found that 40 percent of people said the quality of care had gotten worse in the past five years, while 17 percent said the quality had gotten better and 38 percent said it had stayed the same.
There are many different types of medical errors that can occur in all different types of facilities. Reducing the number of medical errors and improving the response to errors is the number one goal. Much work remains to be done and there is still much to be learned but the important issue is that systems, process improvements and recommendations are now being set into place (Vantage Professional Education, 2006).
Doctors being human, the public need to empathize with them for errors that could be made. But it is well within their command to reduce such errors to minimal levels. Firstly, new technology that could significantly alleviate probability of errors need to be evidenced. However, till such time such errors are sought out and permanently decreased, these would continue to be main areas of medical care.
Summary, Conclusion, Recommendations
Summary
The purpose of this research is to determine ways to create a safer work environment and awareness of safety practices among employees. Physicians play a vital role in reducing the prevalence of medical errors. Physicians should provide leadership to make patient safety a priority and to increase staff awareness of potential patient safety threats.
The problem statement dealt with the high cost of malpractice insurance premiums. Since the 90’s the nation’s health care bill has added $7 billion to the cost. The information received from the Institute of Medicine stated that by 2010 there should be a 50% reduction in medication errors. The continuation of committee reviews, implementing policy and procedures, checks and balances, education, and effective communication can avoid diagnostic errors. In order to achieve these goals, much work lies ahead.
It is evidenced that of the 20 health care providers (Risk Managers) who were chosen for the survey, only 18 of them actually participated in the scheme. Most of the respondents were similar, in that, considering the present health care environment, the rate of medical malpractices was overwhelming and need to be sufficiently contained if health care is to improve dramatically in the 21st Century. Moreover, it is also seen that, according to most risk managers, there is need for robust legislation and its implementation in the area of risk management, and there also needs to be mandatory laws for risk management in health care settings if the interests of patients and their treatment are to be improved and enhanced from the present state.
There is need for trusted methods to be developed and enforced that could consider the impact of medial malpractices in the present state, and ways and means need to be developed that could enhance patient service and caring, both in qualitative and quantitative terms. There is need for utmost trust and confidence to be exercised from both sides, in order to foster an environment of risk management and its smooth and effective transition into the administrative health care functioning of care centers.
In the event risk management is not given the due importance, even a single incident of medical malpractice could considerably encroach upon the financial viability, goodwill and prospects of health care institutions. The depletion of financial assets by way of damages and penalties, indulging in litigation aside, it would have far reaching implications on the authenticity and reputation of the institution.
Moreover, it could also compromise on the faith and reliance placed by patients and their careers, insurance companies, underwriters and a host of other intermediaries and firms that do business with such institutions. Thus, it is very important and intrinsic that health care institutions, however small they may be, need to have a robust and pro-active risk management system in place, not only to safeguard the assets of the institution from being frittered away in long and expensive legal cases, but more significantly, to protect the best interests of the customers, clients and patients who are depending upon them in more ways than one.
The outcome of the deliberations with risk manager respondents also reinforced the fact that two-way communicating system between provider and patient is very important, and underpins the degree of trust and confidence each places on the other for the safe delivery of services and the right attitude to getting well.
The respondents were unanimous on the fact that gaps in provider-patient communication could delay the recovery process and add severe strain to their association. This is more pronounced in geriatric care and emergency room care (ICU/ICCU units) where a round-the-clock surveillance and vigilance in terms of patient care is critically necessary. It could also be in terms of informed consent of patient to medical interventions that are needed, and it is necessary that she/he is aware of and fully consenting to such interventions. According to the respondents, the aspect of medical negligence, or medical malpractices could be proceeded, if there has been a lack of care, or enforcement of medical ethics in attending to patients in health care settings.
Legal proceedings could be established and enforced if it is proved that there has been lack of care which resulted in loss or injury to the patients directly attributable to the service provided by health care delivery systems. In the event of lack of communication, it is not certain whether a patient could get the benefits of informed counsel and medication that is so necessary for his well being and ultimate recovery. Providers on their part would also stand exposed to the possibilities of lowered degree of care and its legal connotations in terms of injury, or even death of patients.
Conclusions
Health care risk management is a process to be practiced by medical staff and other employees on a daily basis. The basis to this practice is through disallowing the occurrences of incidents. Pro-active dedication endeared by medical staff as well as unflinching loyalty is critical ingredients for the success of health care management programs. Every subsection is liable for disallowing dangers and controlling risks within its parameters.
With the cost of professional medical malpractice liability rising significantly, managing the complex issues of risk and patient safety is becoming increasingly important. Unmanaged litigation and insurance, increases in clinical exposure, variance in medical care and inadequate support systems offer some explanations to the increased costs (Risk Management Foundation of the Harvard Institutions, Inc., 2003).
The challenges have never been greater, the work force never smaller, the technology more complicated, the patient’s demand never higher. Despite all these tensions, healthcare professionals and those who assist them in managing the risks associated with their responsibilities must continue to remember that, every day patients and their families entrust their lives to them. Physicians owe it to their patient to be worthy of that trust.
Most healthcare risk managers look forward to the opportunities ahead and are dedicated to managing their organization’s risk and enhancing patient safety. The future is fraught with peril and great risk but also great reward. Those risk managers who accept change and think of new ways to embed risk management principles into their organizations to help create meaningful and sustainable change will prosper. Those who don’t should get out now.
Medical malpractice and malpractice insurance continue to be issues of great concern to physicians, consumers, legislators, and others. Much of the deliberations about increasing malpractice insurance premium have focused upon limiting the damage awards in malpractice cases and some thoughts have been fostered on need for reforms in the insurance sector. Another concern that has received less public notice in malpractice discussions of recent years is patient safety. Safety of patients refers to the gamut of rules, practices and systems that govern the need to circumvent medical injuries, and the stratagems to obstruct medical mistakes need to be imbued in norms of patient welfare. Increasing medical malpractice insurance premiums are a growing concern in the American healthcare system. Many physicians, professional organization, and lawmakers claim that the tort system encourages frivolous law suits and jackpot verdicts. In order to prevent a major dearth in healthcare access, strict malpractice liability restrictions, including caps on non-economic damages must be mandated.
It is unlikely that an acceptable, comprehensive resolution of the malpractice problem will be easily found. But if reform of our health care system is to become reality, and it should, the federal government must recognize the failures of past state action and act as a catalyst through federal legislation to contain and make a more rational system that is now slow, expensive, and inequitable. The success of health care reform is too important to be threatened by a failure to recognize and remedy the deficiencies of our malpractice system, which now constitute a barrier to the reform of the system as a whole (New England Journal of Medicine, 1993).
Physicians need to find a way to make their perspective on quality measurement and improvement. They cannot accomplish this without new skills, attitudes, and partners. The success of physicians in acquiring these resources, and in avoiding entanglements that divide them from their patients, will powerfully affect the future both of the profession and of quality measurement and improvement in the U.S. health care system (New England Journal of Medicine, 1996).
A transformation in how the medical profession communicates with patients about harmful medical errors has begun. Within a decade, full and frank disclosure of these events to patients is likely to be the norm rather than the exception. Making disclosure of harmful errors to patients and expectation in medicine and giving providers the tools to turn this principle into practice may prove to be critical step in restoring the public’s trust in the honesty and integrity of the health care system (New England Journal of Medicine, 2007).
Risk Management symbolizes an ever moving procedure in a health delivery system that can result in improved patient care and reduced accountability. Important mechanism of the process includes nurturing a good relationship with the patient, obtaining approval after appraising all facts, practicing within established guidelines, and careful documentation. A triumphant risk management program can also cause fruitful Continuous Quality Improvement plan. An efficient risk management practice does not ignore risks. Having an effectual and operational risk management shows an insurer that your business is devoted to loss decreasing or elimination. It builds a better risk insurance mechanism into your organization.
Risk management basically involves policies, process, and procedures that identify potential operational and financial losses, prevent losses whenever possible and lessen the effects of losses that cannot be prevented. Some of the steps that are involved with risk management are identifying and analyzing potential risks, preventing and reducing the effects of accidents, medical errors and other injuries and losses. Risk management must include a heightened sensitivity to provide a safe environment and addressing the emotional needs of patients. Good relationships with patients are very important in preventing malpractice suits. Public relations for health care professionals are a challenge. It is not only good medical practice but it is at the very core of the problem of medical malpractice.
Risk management is primarily designed to protect the financial assets of an organization by assuring adequate financial protection against potential liability through appropriate insurance coverage. The goal to risk management planning is to decrease the probability of identified negative risks. This can be accomplished by inserting resources into the budget plan.
Recommendations
From the deliberations with health risk managers and their views on the aspects of risk management, it is abundantly clear that there needs to be a sound and plausible health care management system that could address all facets of patient-provider caring and also create a congenial and positive health care environment that could enhance patient treatment and early recovery.
Moreover, it is seen that in the current settings, it is important that a cohesive and well structured risk management plan, addressing all major areas of public health accountability and patient care, irrespective of the specifics of the case and local influences, need to be formulated and executed to save future litigation and redundant health care costs. Thus, “all health care providers must focus on enhancing the effectiveness of their risk management programs.” (Effective health care risk management programs, n.d., p.8) Those who are unable to do so would definitely be marginalized for failing to provide suitable patient safety protections and would surely find insurance coverage for professional liabilities and injuries difficult to obtain and enforce.
Thus, it is not only in the best interest of the patients but also that of the provider institution to enforce a disciplined and well rounded risk management policy that could possibly attend to all areas of patient care and its implications on the accidental aspects of health care business. Providers who neglect or undermine such schemes may be seriously disadvantaged over time and may find themselves in deeper quagmire than before.
In order for the Risk Management Program to remain successful the researcher also recommends the following:
- Create National Center for Patient Safety.
- Develop error reporting system which must guarantee confidentiality.
- Raise performance standards and commitment to safety within professional groups and accreditation boards.
- Implement safety standards at the patient delivery level.
Reference List
Abdelhak, M. (1996). Health information: management of a strategic resource. Philadelphia, PA: W.B. Saunders Company.
Bellandi, D. (1997). The expanding reach of risk management. Modern Healthcare, 27 (43), 56-7, 57.
Bleier, R.A. (2004). Risk prevention means teamwork. Nursing Homes. Cleveland. 53(10), 74, 1.
Dulworth, S. (2003). Commentary: Exploiting the overlap: Using utilization management to reduce medical malpractice. American Journal of Medical Quality, 18(3), 128-132. Sage Journal Online. Web.
Effective health care risk management programs: Components for success: Conclusion. (n.d.). Chubb Health Care. 8.
Huffman, E. K. (1990). Medical record management. Berwyn, IL: Physicians Record Company.
Johns, M.L. (2002). Health information management technology. Chicago, IL: American Health Information Management Association.
Kemshall, H., & Pritchard, J. (Eds.). (1996). Good practice in risk assessment and risk management. Bristol, PA. Jessica Kingsley.
McGinnis, J., Risk management strategies for an integrated health care delivery system. QRC Advisor, 1999; 15(7), 1-8, 5.
Medical malpractice jury trial verdicts (2008). (n.d.). Web.
Sentinel event statistics as of: 2009. (n.d.). The Joint Commission. Web.
Showalter, Stuart J. (2004). The law of healthcare administration. Chicago, IL: Health Administration Press.
Wells Fargo Healthcare: Operational risk management & safety assessment. (n.d.). 2009 WFIS Operational Risk Management & Safety Assessment.
Youngberg, B.J. (1990). Essential of hospital risk management. Rockville, MD: Aspen Publishers.
Youngberg, B.J. (1994). The risk manager’s desk reference. Gaithersburg, MD: Aspen Publication.
Appendix 1
Appendix 2